2023 might be the worst tick season ever. The CDC has comprehensive guidelines on how to avoid tickers on people, on pets, in the yard; how to remove ticks; how to check symptoms (and when to see a doctor); where ticks live; how to identify a tick; etc. In this article, we summarized all the information from the CDC; we also added where to get the products recommended in the guidelines.
Avoid ticks on people
Tick exposure can occur year-round, but ticks are most active during warmer months (April-September).
Before you go outdoors
- Know where to expect ticks. Ticks live in grassy, brushy, or wooded areas, or even on animals. Spending time outside walking your dog, camping, gardening, or hunting could bring you in close contact with ticks. Many people get ticks in their own yard or neighborhood.

- Treat clothing and gear with products containing 0.5% permethrin. Permethrin can be used to treat boots, clothing and camping gear and remain protective through several washings. Alternatively, you can buy permethrin-treated clothing and gear.


- Use EPA-registered insect repellentsexternal containing DEET, picaridin, IR3535, Oil of Lemon Eucalyptus (OLE), para-menthane-diol (PMD), or 2-undecanone. EPA’s helpful search toolexternal icon can help you find the product that best suits your needs. Always follow product instructions. Do not use products containing OLE or PMD on children under 3 years old.
Active ingredient: DEET 25%
Active ingredient: 20% Picaridin

- Avoid Contact with Ticks. Avoid wooded and brushy areas with high grass and leaf litter. Walk in the center of trails.
Keeps ticks out when hiking
After you come indoors
Check your clothing for ticks. Ticks may be carried into the house on clothing. Any ticks that are found should be removed. Tumble dry clothes in a dryer on high heat for 10 minutes to kill ticks on dry clothing after you come indoors. If the clothes are damp, additional time may be needed. If the clothes require washing first, hot water is recommended. Cold and medium temperature water will not kill ticks.
Examine gear and pets. Ticks can ride into the home on clothing and pets, then attach to a person later, so carefully examine pets, coats, and daypacks.
Shower soon after being outdoors. Showering within two hours of coming indoors has been shown to reduce your risk of getting Lyme disease and may be effective in reducing the risk of other tickborne diseases. Showering may help wash off unattached ticks and it is a good opportunity to do a tick check.
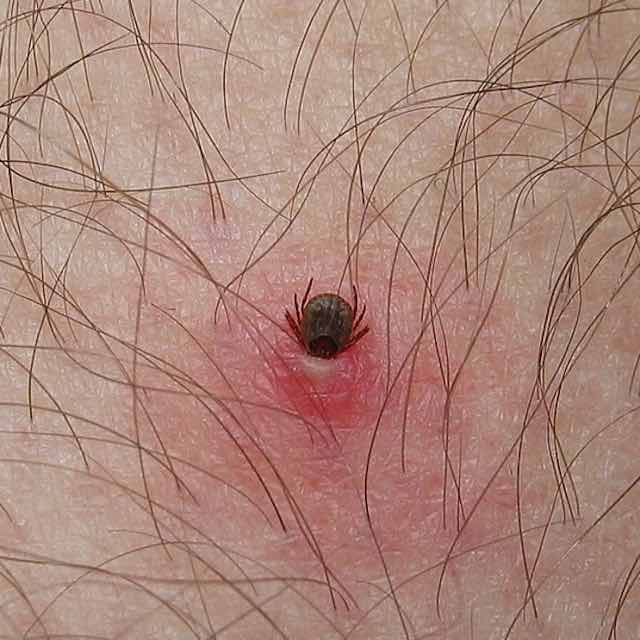 Image: Denys Williams Image: Denys Williams |  Image: NIAID Image: NIAID |
 Image: Tomfy Image: Tomfy | 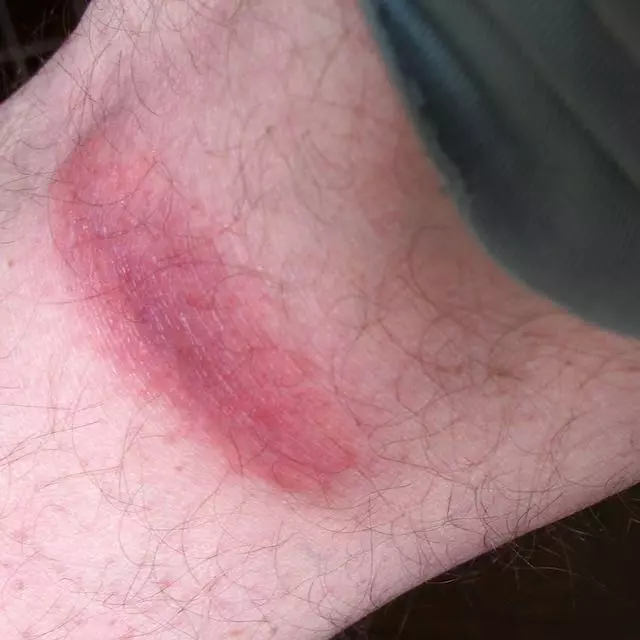 Image: Túrelio Image: Túrelio |
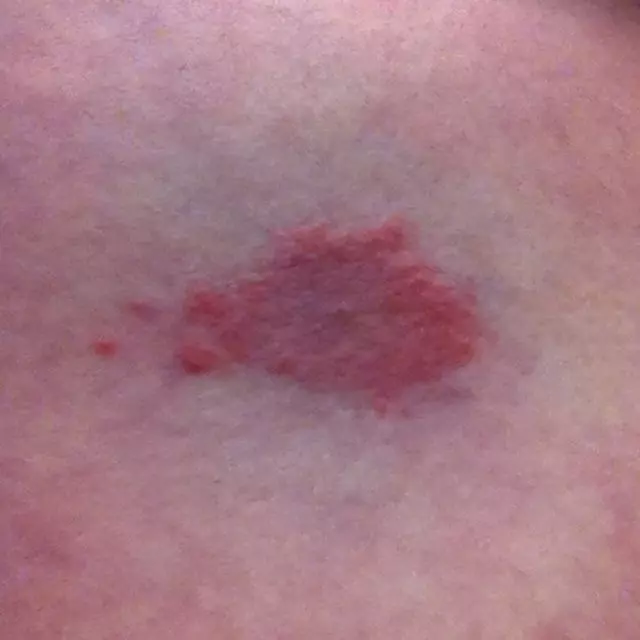 Image: Just Some Guy Image: Just Some Guy | 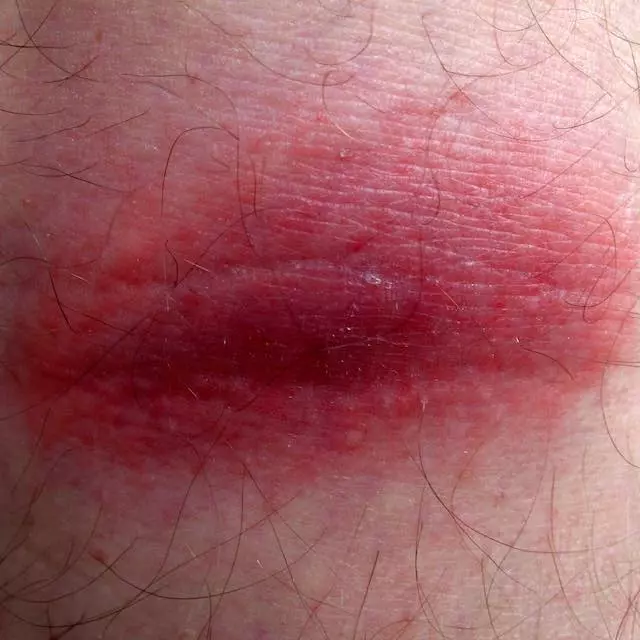 Image: Túrelio Image: Túrelio |
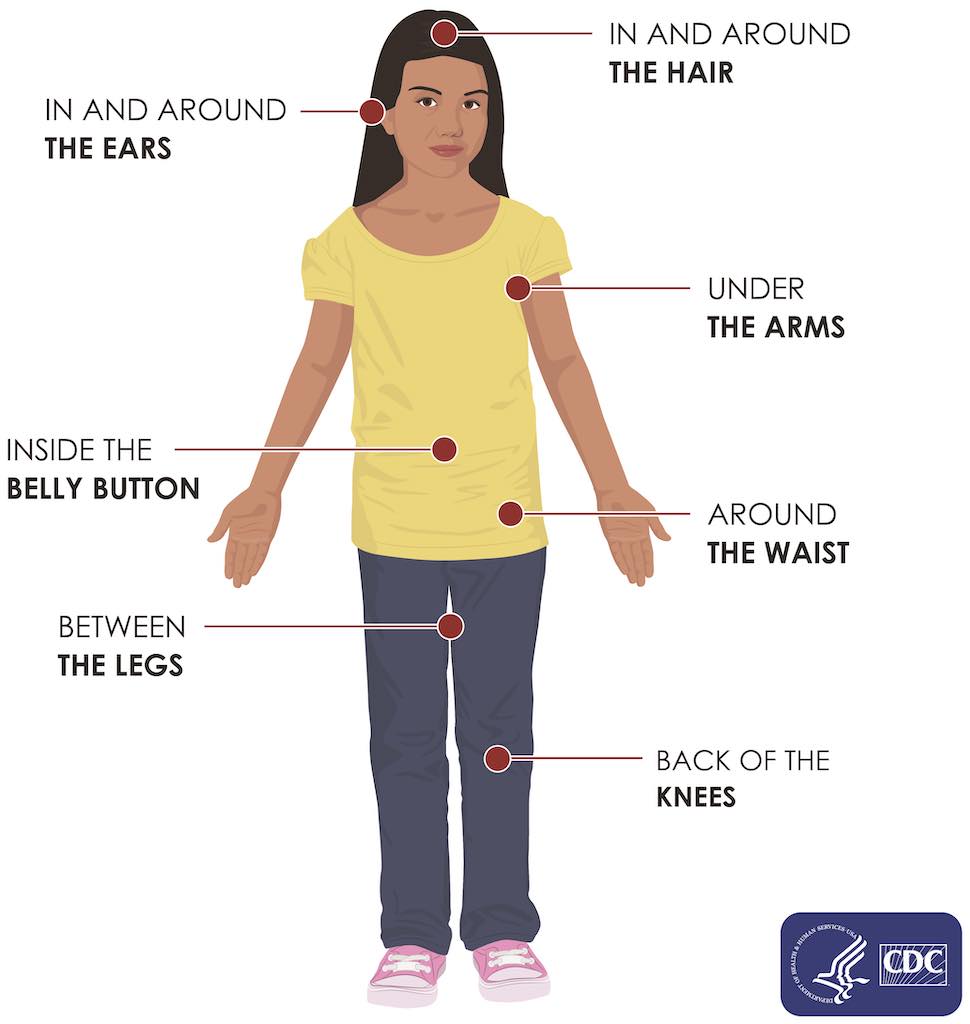
Check your body for ticks after being outdoors. Conduct a full body check upon return from potentially tick-infested areas, including your own backyard. Use a hand-held or full-length mirror to view all parts of your body. Check these parts of your body and your child’s body for ticks:
- Under the arms
- In and around the ears
- Inside belly button
- Back of the knees
- In and around the hair
- Between the legs
- Around the waist
Avoid ticks on your pets
Dogs are very susceptible to tick bites and tickborne diseases. Vaccines are not available for most of the tickborne diseases that dogs can get, and they don’t keep the dogs from bringing ticks into your home. For these reasons, it’s important to use a tick preventive product on your dog.

For small dogs 8 months protection | For large dogs 8 months protection |
Tick bites on dogs may be hard to detect. Signs of tickborne disease may not appear for 7-21 days or longer after a tick bite, so watch your dog closely for changes in behavior or appetite if you suspect that your pet has been bitten by a tick.

Flea & tick treatment For small dogs | Flea & tick treatment For large dogs |
Talk to your veterinarian about:
- The best tick prevention products for your dog
- Tickborne diseases in your area
To further reduce the chances that a tick bite will make your dog sick:
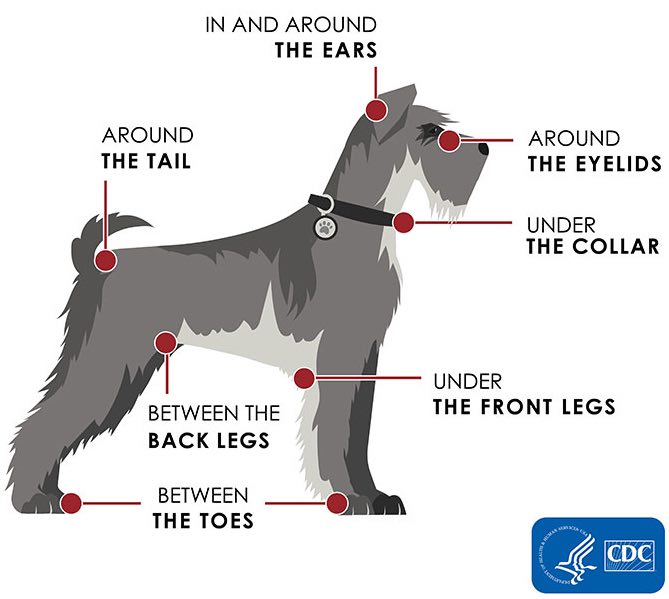
- Check your pets for ticks daily, especially after they spend time outdoors.
- If you find a tick on your pet, remove it right away.
- Reduce tick habitat in your yard.
Cats are extremely sensitive to a variety of chemicals. Do not apply any tick prevention products to your cats without first asking your veterinarian!
Prevent ticks in your yard
Use of pesticides can reduce the number of ticks in treated areas of your yard. However, you should not rely on spraying to reduce your risk of infection.
Treats up to 5,000 Sqf
When using pesticides, always follow label instructions. Before spraying, check with local health or agricultural officials about:
- The best time to apply pesticide in your area
- The best type of pesticide to use
- Rules and regulations regarding pesticide application on residential properties
The Connecticut Agricultural Experiment Station has developed a comprehensive Tick Management Handbook for preventing tick bites. Here are some simple landscaping techniques that can help reduce blacklegged tick populations:
- Remove leaf litter.
- Clear tall grasses and brush around homes and at the edge of lawns.
- Place a 3-ft wide barrier of wood chips or gravel between lawns and wooded areas to restrict tick migration into recreational areas.
- Mow the lawn frequently.
- Stack wood neatly and in a dry area (discourages rodents).
- Keep playground equipment, decks, and patios away from yard edges and trees.
- Discourage unwelcome animals (such as deer, raccoons, and stray dogs) from entering your yard by constructing fences.
- Remove old furniture, mattresses, or trash from the yard that may give ticks a place to hide.
Self care of tick bites
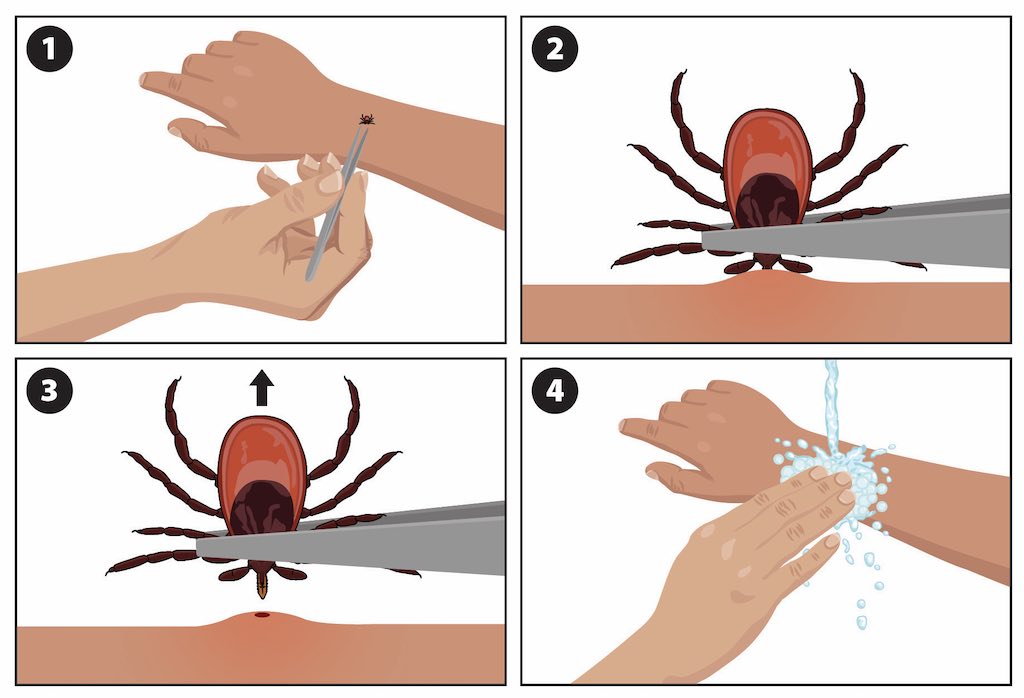
If you find a tick attached to your skin, simply remove the tick as soon as possible. There are several tick removal devices on the market, but a plain set of fine-tipped tweezers works very well.
- Use clean, fine-tipped tweezers to grasp the tick as close to the skin’s surface as possible.
- Pull upward with steady, even pressure. Don’t twist or jerk the tick; this can cause the mouth-parts to break off and remain in the skin. If this happens, remove the mouth-parts with tweezers. If you cannot remove the mouth easily with tweezers, leave it alone and let the skin heal.
- After removing the tick, thoroughly clean the bite area and your hands with rubbing alcohol or soap and water.
- Never crush a tick with your fingers. Dispose of a live tick by
- Putting it in alcohol,
- Placing it in a sealed bag/container,
- Wrapping it tightly in tape, or
- Flushing it down the toilet.
You can take below measures to care for yourself at home:
- Put ice or a cold pack on the bite for 15 to 20 minutes once an hour.
- Try an over-the-counter medicine to relieve itching, redness, swelling, and pain.
- Take an antihistamine medicine to help relieve itching, redness, and swelling.
- Use a spray of local anesthetic that contains benzocaine. It may help relieve pain. If your skin reacts to the spray, stop using it.
- Put calamine lotion on the skin. It may help relieve itching.
Pain & itch relief spray Benzocaine 20% Menthol 0.5% | 6 fl oz / 177 ml Pain & itch relief |
Should I see the doctor?
Many tickborne diseases can have similar signs and symptoms. If you get a tick bite and develop the symptoms below within a few weeks, see your healthcare provider. The most common symptoms of tick-related illnesses include:
- Fever/chills. All tickborne diseases can cause fever.
- Aches and pains. Tickborne diseases can cause headache, fatigue, and muscle aches. People with Lyme disease may also have joint pain.
- Rash. Lyme disease, Southern tick-associated rash illness (STARI), Rocky Mountain spotted fever (RMSF), ehrlichiosis, and tularemia can cause distinctive rashes.
Your healthcare provider should evaluate the following before deciding on a plan for treatment:
- Your symptoms,
- the geographic region where you were bitten, and
- lab tests, depending on the symptoms and the geographic region where you were bitten.
Treatment for tickborne diseases should be based on symptoms, history of exposure to ticks, and in some cases, blood test results. Most tickborne diseases can be treated with a short course of antibiotics.
In general, CDC does not recommend taking antibiotics after tick bites to prevent tickborne diseases. However, in certain circumstances, a single dose of doxycycline after a tick bite may lower your risk of Lyme disease. Consider talking to your healthcare provider if you live in an area where Lyme disease is common.
Should I test the tick?
People who have removed a tick sometimes wonder if they should have it tested for evidence of infection. Although some commercial groups offer testing, in general this is not recommended because:
- Laboratories that conduct tick testing are not required to have the high standards of quality control used by clinical diagnostic laboratories. Results of tick testing should not be used for treatment decisions.
- Positive results showing that the tick contains a disease-causing organism do not necessarily mean that you have been infected.
- Negative results can lead to false assurance. You may have been unknowingly bitten by a different tick that was infected.
- If you have been infected, you will probably develop symptoms before results of the tick test are available. If you do become ill, you should not wait for tick testing results before beginning appropriate treatment.
However, you may want to learn to identify various ticks. Different ticks live in different parts of the country and transmit different diseases.
Regions where ticks live
Of the many different tick species found throughout the world, only a select few bite and transmit bacteria, viruses, and parasites, or pathogens, that cause diseases in people. Of the ticks that bite people, different species of ticks transmit different pathogens. These maps show the general distribution of medically important human-biting ticks in the contiguous United States. Populations of ticks may be found outside shaded areas. Naturally occurring populations of the ticks described below do not occur in Alaska; however, the brown dog tick occurs in Hawaii.

The two ticks in the picture are both females. The one on the left is a hard tick, and the adult has a strongly calcified shield on the back of its body. The one on the right is a soft tick, with no shield on the back of its body. Its body surface is often covered with granular small nodules or wrinkles and depressions. Adult ticks are 2-10mm long and are about the size of a green bean when unfed. After a blood meal, the size of the tick can increase several times or even tens of times.
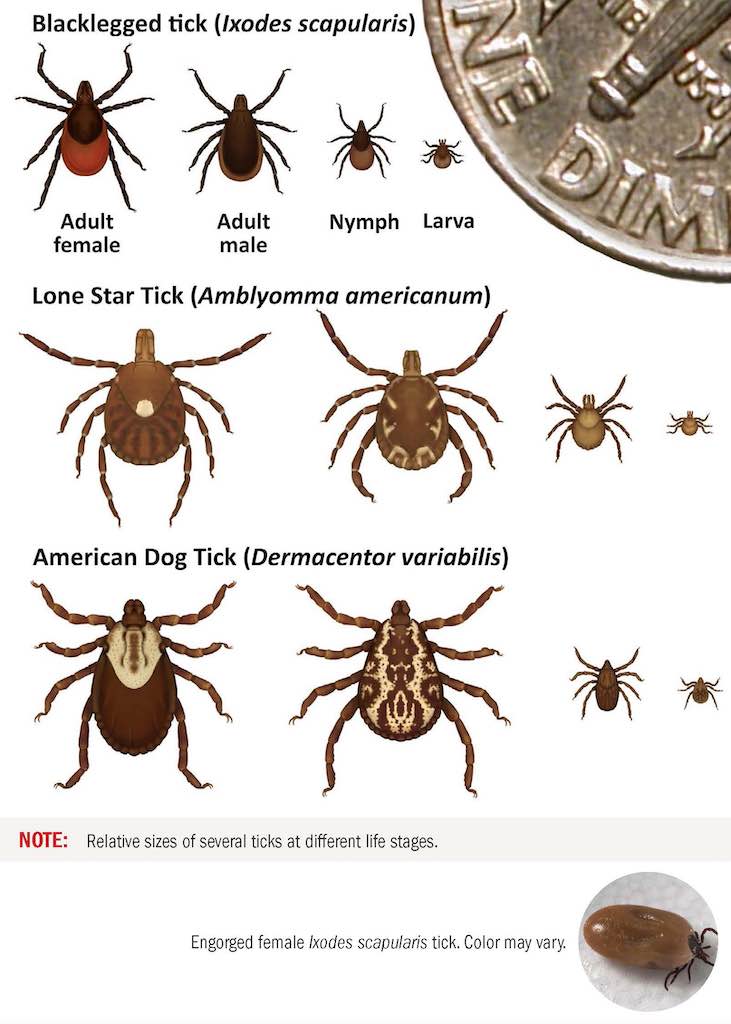
Note that adult ticks are the easiest to identify and male and female ticks of the same species may look different. Nymphal and larval ticks are very small and may be hard to identify. Below are the common ticks in the U.S. and the first three are the most common ones to bite humans.
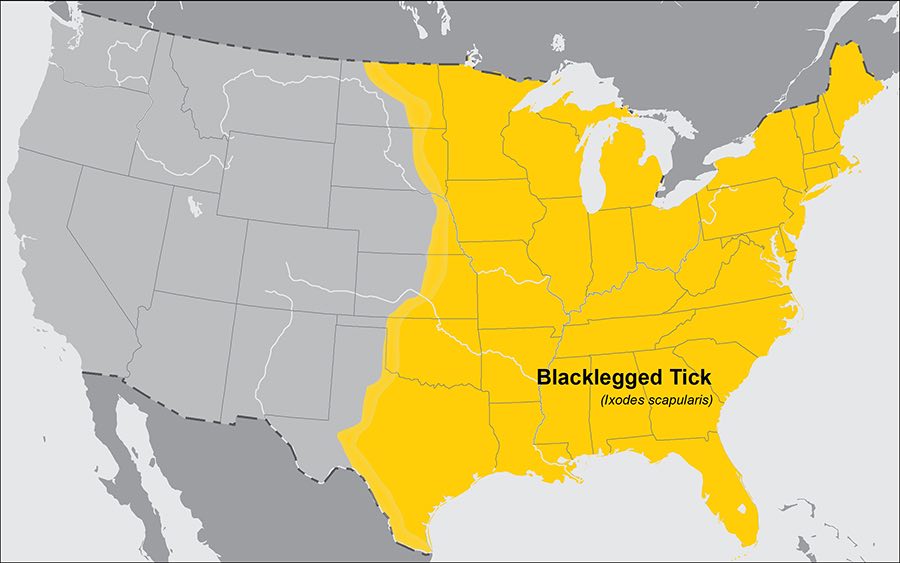
Blacklegged Tick (Ixodes scapularis)

- Where found: Widely distributed across the eastern United States.
- Transmits: Borrelia burgdorferi and B. mayonii (which cause Lyme disease), Anaplasma phagocytophilum (anaplasmosis), B. miyamotoi (hard tick relapsing fever), Ehrlichia muris eauclairensis (ehrlichiosis), Babesia microti (babesiosis), and Powassan virus (Powassan virus disease).
- Comments: The greatest risk of being bitten exists in the spring, summer, and fall. However, adults may be out searching for a host any time winter temperatures are above freezing. Stages most likely to bite humans are nymphs and adult females.
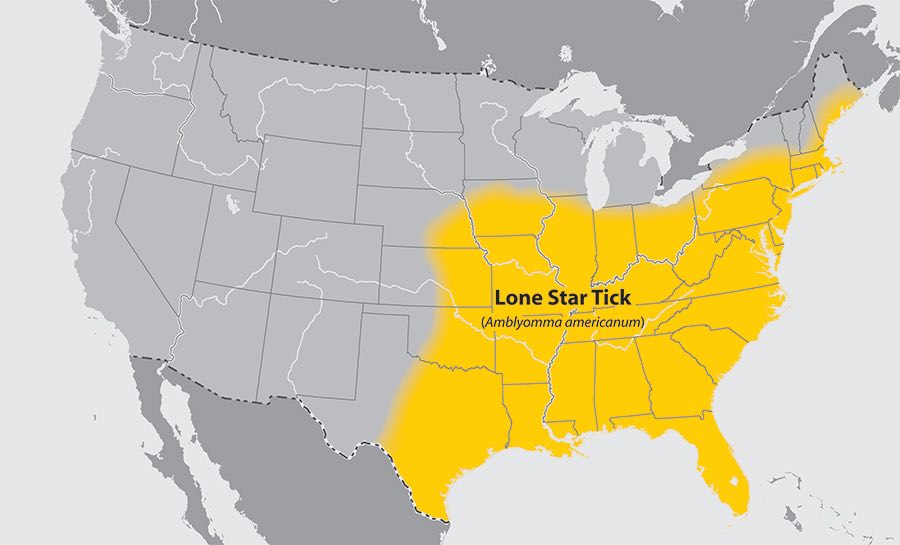
Lone star tick (Amblyomma americanum)

- Where found: Widely distributed in the eastern, southeastern, and south-central United States.
- Transmits: Bourbon virus, Ehrlichia chaffeensis and Ehrlichia ewingii (which cause human ehrlichiosis), Heartland virus, tularemia, and STARI. Growing evidence suggests that alpha-gal syndrome (red meat allergy) may be triggered by the bite of lone star ticks; however, other tick species have not been ruled out.
- Comments: A very aggressive tick that bites humans. The adult female is distinguished by a white dot or “lone star” on her back. Lone star tick saliva can be irritating; redness and discomfort at a bite site does not necessarily indicate an infection. The nymph and adult females most frequently bite humans and transmit disease.
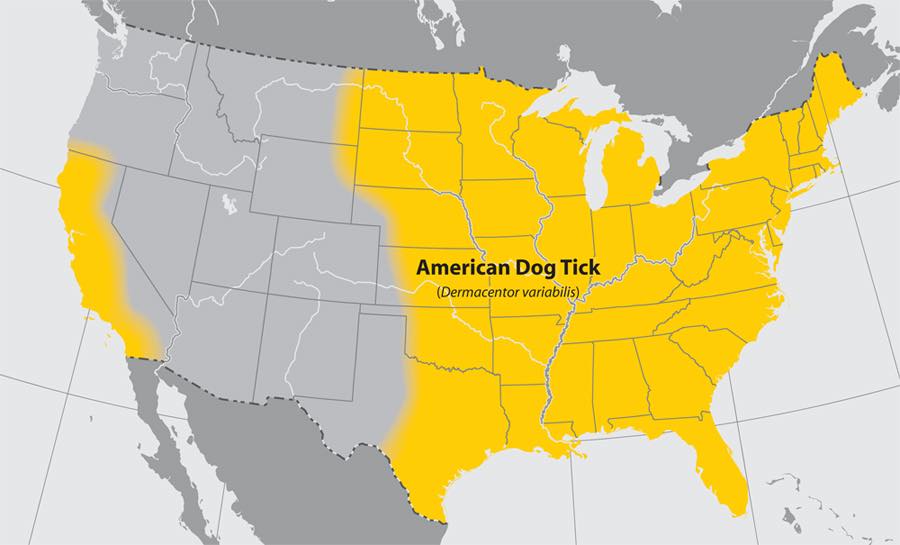
American Dog Tick (Dermacentor variabilis, D. similis)

- Where found: D. variabilis is widely distributed east of the Rocky Mountains. Also occurs in limited areas on the Pacific . Newly described D. similis is found west of the Rocky Mountains. More research is needed to understand the role of these species in disease transmission.
- Transmits: Tularemia and Rocky Mountain spotted fever.
- Comments: The highest risk of being bitten occurs during spring and summer. Adult females are most likely to bite humans.
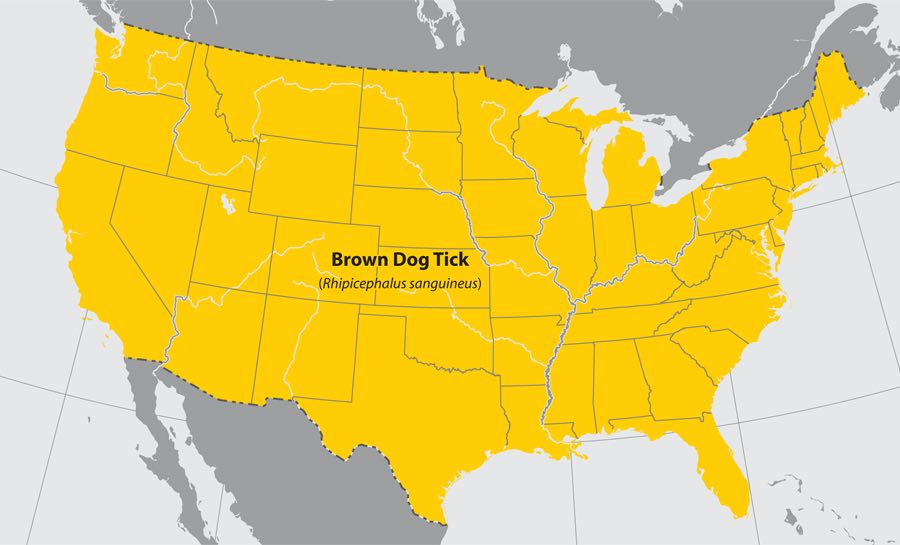
Brown dog tick (Rhipicephalus sanguineus)

- Where found: Worldwide.
- Transmits: Rocky Mountain spotted fever (in the southwestern U.S. and along the U.S.-Mexico border).
- Comments: Dogs are the primary host for the brown dog tick in each of its life stages, but the tick may also bite humans or other mammals.
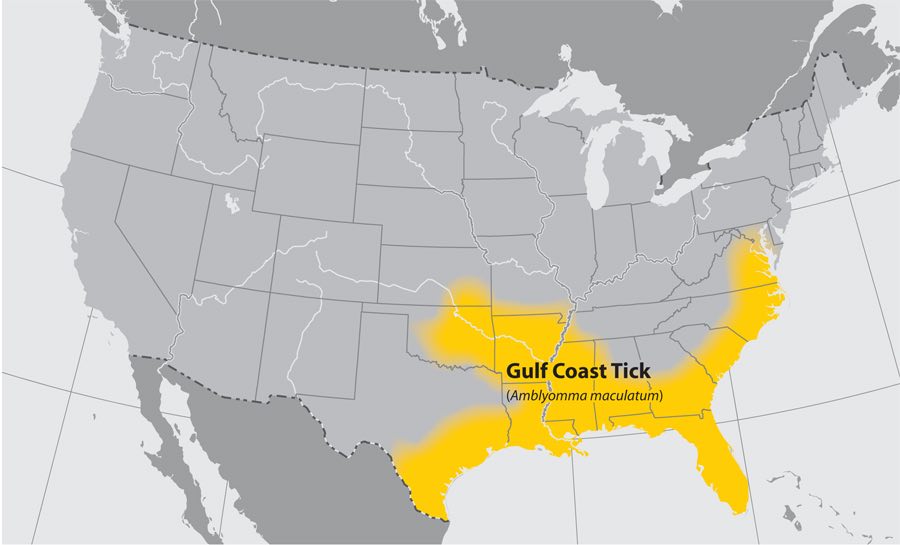
Gulf Coast tick (Amblyomma maculatum)

- Where found: Coastal areas of the U.S. along the Atlantic coast and the Gulf of Mexico.
- Transmits: Rickettsia parkeri rickettsiosis, a form of spotted fever.
- Comments: Larvae and nymphs feed on birds and small rodents, while adult ticks feed on deer and other wildlife. Adult ticks have been associated with transmission of R. parkeri to humans.
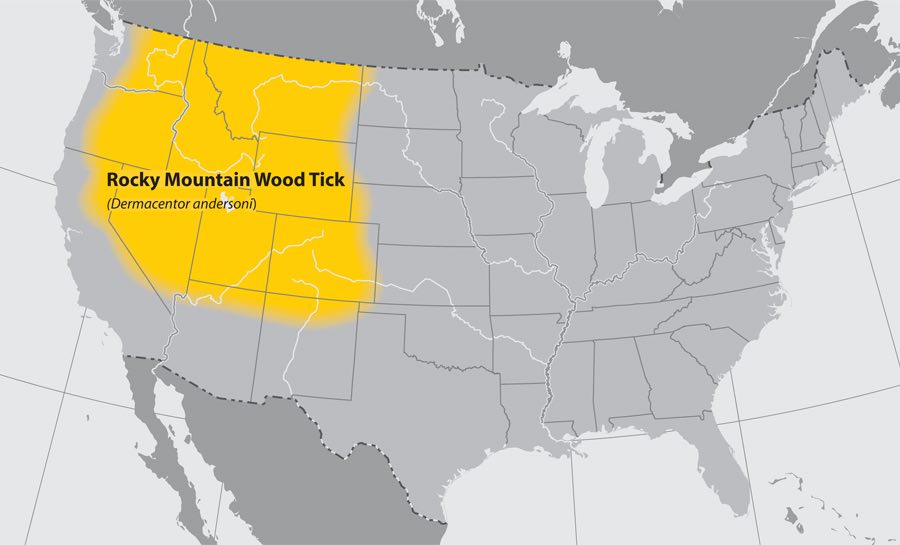
Rocky Mountain wood tick (Dermacentor andersoni)

- Where found: Rocky Mountain states and southwestern Canada from elevations of 4,000 to 10,500 feet.
- Transmits: Rocky Mountain spotted fever, Colorado tick fever, and tularemia.
- Comments: Adult ticks feed primarily on large mammals. Larvae and nymphs feed on small rodents. Adult ticks are primarily associated with pathogen transmission to humans.
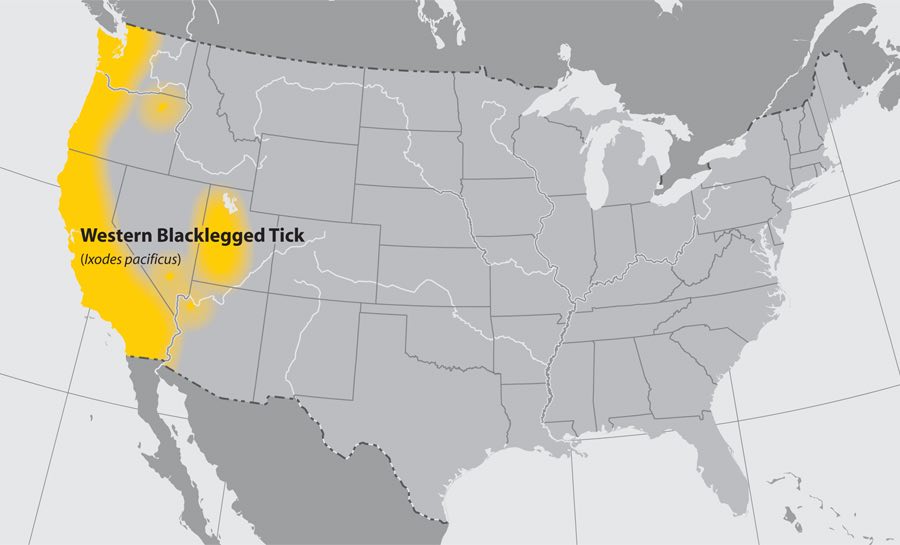
Western blacklegged tick (Ixodes pacificus)

- Where found: Along the Pacific coast of the United States, particularly northern California.
- Transmits: Anaplasma phagocytophilum (anaplasmosis), Borrelia burgdorferi (Lyme disease), and B. miyamotoi (hard tick relapsing fever)
- Comments: Larvae and nymphs often feed on lizards, birds, and rodents, and adults more commonly feed on deer. Although all life stages bite humans, nymphs and adult females are more often reported on humans.
What diseases do ticks spread?
How ticks survive
Most ticks go through four life stages: egg, six-legged larva, eight-legged nymph, and adult. After hatching from the eggs, ticks must eat blood at every stage to survive. Ticks that require this many hosts can take up to 3 years to complete their full life cycle, and most will die because they don’t find a host for their next feeding.

Relative sizes of several ticks at different life stages.
Some tick species, like the brown dog tick, prefer to feed on the same host during all life stages.
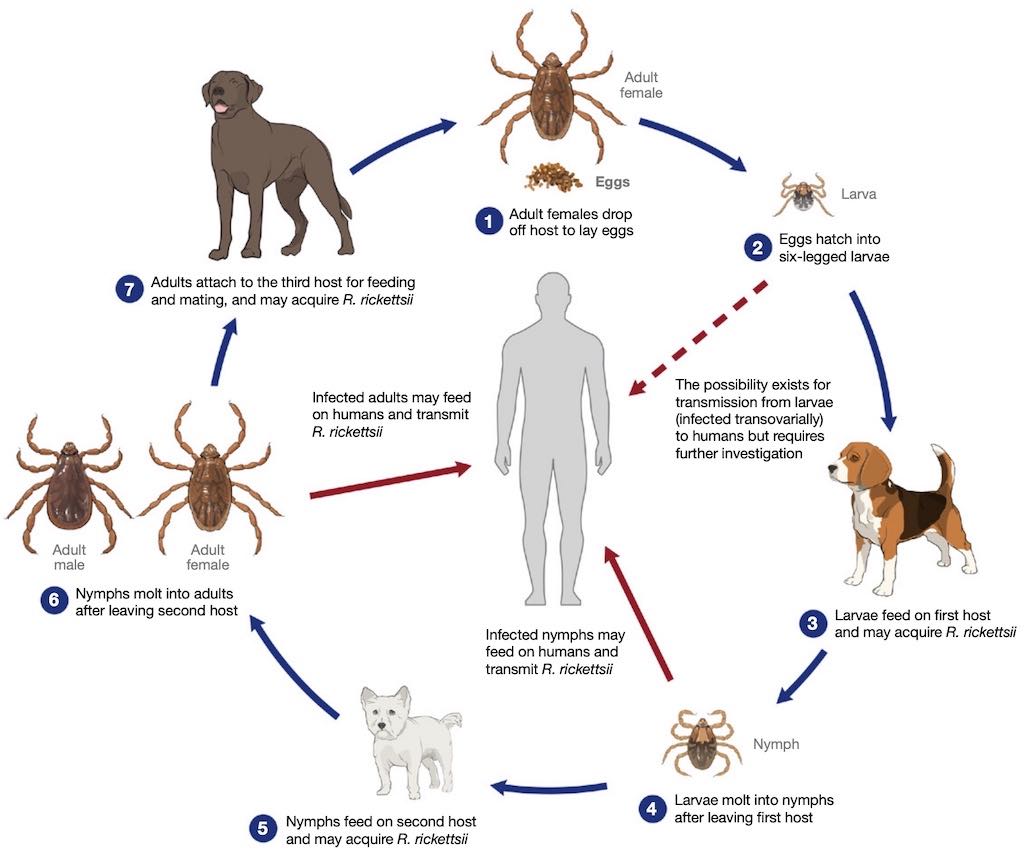
This diagram shows the typical lifecycle of brown dog ticks. Brown dog ticks spread the bacteria that causes Rocky Mountain spotted fever in some parts of the southwestern United States and Mexico.
Ticks can feed on mammals, birds, reptiles, and amphibians. Most ticks prefer to have a different host animal at each stage of their life, as shown below:
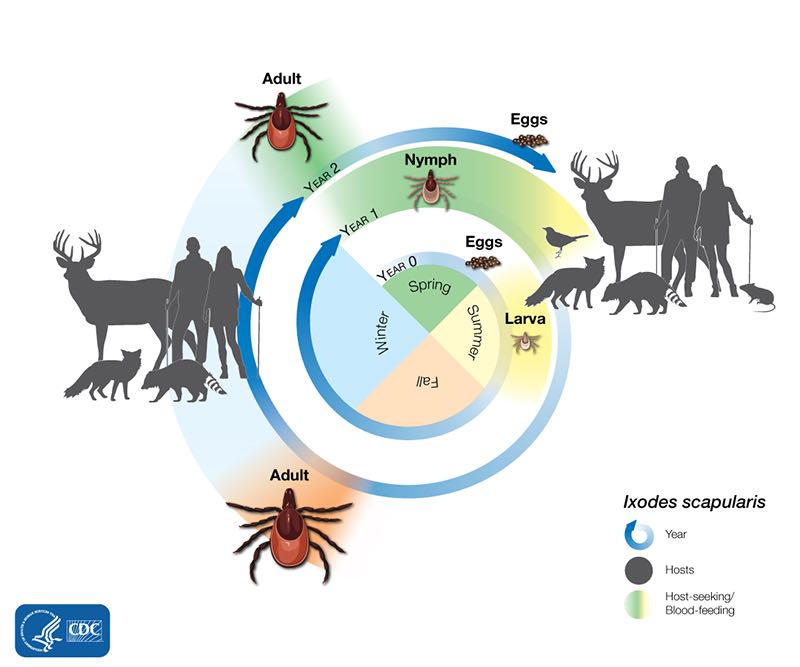
The lifecycle of Ixodes scapularis ticks generally lasts two years. During this time, they go through four life stages: egg, larva, nymph, and adult. After the eggs hatch, the ticks must have a blood meal at every stage to survive. Blacklegged ticks can feed from mammals, birds, reptiles, and amphibians. The ticks need a new host at each stage of their life.
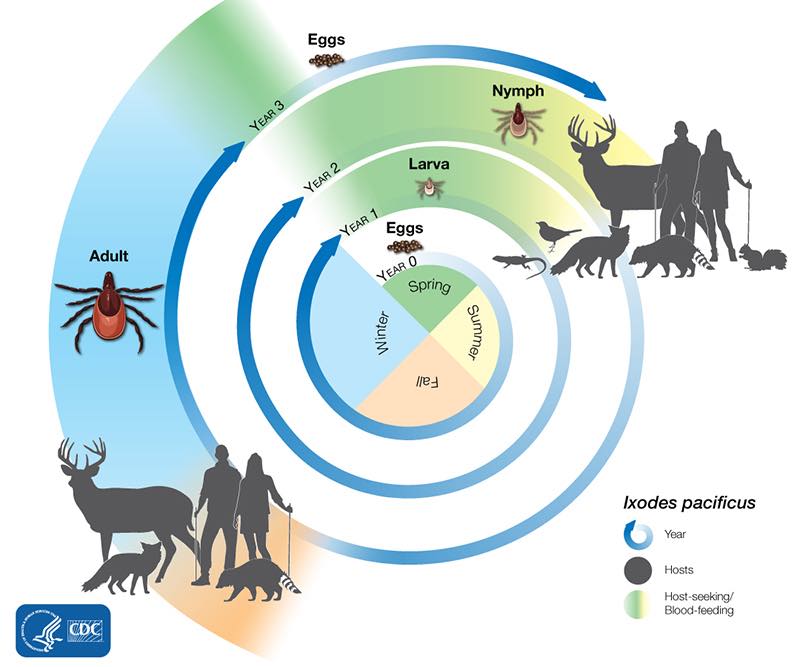
The lifecycle of Ixodes pacificus ticks generally lasts three years. During this time, they go through four life stages: egg, larva, nymph, and adult. After the eggs hatch, the ticks must have a blood meal at every stage to survive. Blacklegged ticks can feed from mammals, birds, reptiles, and amphibians. The ticks need a new host at each stage of their life.
How ticks find their hosts
Ticks find their hosts by detecting animals’ breath and body odors, or by sensing body heat, moisture, and vibrations. Some species can even recognize a shadow. In addition, ticks pick a place to wait by identifying well-used paths. Then they wait for a host, resting on the tips of grasses and shrubs. Ticks can’t fly or jump, but many tick species wait in a position known as “questing”.
While questing, ticks hold onto leaves and grass by their third and fourth pair of legs. They hold the first pair of legs outstretched, waiting to climb on to the host. When a host brushes the spot where a tick is waiting, it quickly climbs aboard. Some ticks will attach quickly and others will wander, looking for places like the ear, or other areas where the skin is thinner.
How ticks spread disease
Ticks transmit pathogens that cause disease through the process of feeding.
- Depending on the tick species and its stage of life, preparing to feed can take from 10 minutes to 2 hours. When the tick finds a feeding spot, it grasps the skin and cuts into the surface.
- The tick then inserts its feeding tube. Many species also secrete a cement-like substance that keeps them firmly attached during the meal. The feeding tube can have barbs which help keep the tick in place.
- Ticks also can secrete small amounts of saliva with anesthetic properties so that the animal or person can’t feel that the tick has attached itself. If the tick is in a sheltered spot, it can go unnoticed.
- A tick will suck the blood slowly for several days. If the host animal has a bloodborne infection, the tick will ingest the pathogens with the blood.
- Small amounts of saliva from the tick may also enter the skin of the host animal during the feeding process. If the tick contains a pathogen, the organism may be transmitted to the host animal in this way.
- After feeding, most ticks will drop off and prepare for the next life stage. At its next feeding, it can then transmit an acquired disease to the new host.
Diseases transmitted by ticks
In the United States, some ticks carry pathogens that can cause human disease, including:
- Anaplasmosis is transmitted to humans by tick bites primarily from the blacklegged tick (Ixodes scapularis) in the northeastern and upper midwestern U.S. and the western blacklegged tick (Ixodes pacificus) along the Pacific coast.
- Babesiosis is caused by microscopic parasites that infect red blood cells. Most human cases of babesiosis in the U.S. are caused by Babesia microti. Babesia microti is transmitted by the blacklegged tick (Ixodes scapularis) and is found primarily in the northeast and upper midwest.
- Borrelia mayonii infection has recently been described as a cause of illness in the upper midwestern United States. It has been found in blacklegged ticks (Ixodes scapularis) in Minnesota and Wisconsin. Borrelia mayonii is a new species and is the only species besides B. burgdorferi known to cause Lyme disease in North America.
- Borrelia miyamotoi infection has recently been described as a cause of illness in the U.S. It is transmitted by the blacklegged tick (Ixodes scapularis) and has a range similar to that of Lyme disease.
- Bourbon virus infection has been identified in a limited number patients in the Midwest and southern United States. At this time, we do not know if the virus might be found in other areas of the United States.
- Colorado tick fever is caused by a virus transmitted by the Rocky Mountain wood tick (Dermacentor andersoni). It occurs in the the Rocky Mountain states at elevations of 4,000 to 10,500 feet.
- Ehrlichiosis is transmitted to humans by the lone star tick (Ambylomma americanum), found primarily in the southcentral and eastern U.S.
- Heartland virus cases have been identified in the Midwestern and southern United States. Studies suggest that Lone Star ticks can transmit the virus. It is unknown if the virus may be found in other areas of the U.S.
- Lyme disease is transmitted by the blacklegged tick (Ixodes scapularis) in the northeastern U.S. and upper midwestern U.S. and the western blacklegged tick (Ixodes pacificus) along the Pacific coast.
- Powassan disease is transmitted by the blacklegged tick (Ixodes scapularis) and the groundhog tick (Ixodes cookei). Cases have been reported primarily from northeastern states and the Great Lakes region.
- Rickettsia parkeri rickettsiosis is transmitted to humans by the Gulf Coast tick (Amblyomma maculatum).
- Rocky Mountain spotted fever (RMSF) is transmitted by the American dog tick (Dermacentor variabilis), Rocky Mountain wood tick (Dermacentor andersoni), and the brown dog tick (Rhipicephalus sangunineus) in the U.S. The brown dog tick and other tick species are associated with RMSF in Central and South America.
- STARI (Southern tick-associated rash illness) is transmitted via bites from the lone star tick (Ambylomma americanum), found in the southeastern and eastern U.S.
- Tickborne relapsing fever (TBRF) is transmitted to humans through the bite of infected soft ticks. TBRF has been reported in 15 states, including Arizona, California, Colorado, Idaho, Kansas, Montana, Nevada, New Mexico, Ohio, Oklahoma, Oregon, Texas, Utah, Washington, and Wyoming and is associated with sleeping in rustic cabins and vacation homes.
- Tularemia is transmitted to humans by the dog tick (Dermacentor variabilis), the wood tick (Dermacentor andersoni), and the lone star tick (Amblyomma americanum). Tularemia occurs throughout the U.S.
- 364D rickettsiosis (Rickettsia phillipi, proposed) is transmitted to humans by the Pacific Coast tick (Dermacentor occidentalis ticks). This is a new disease that has been found in California.
Learn to identify ticks
Ticks that commonly bite humans are the first three, marked as red.
 | Blacklegged Tick
|
 | Lone Star Tick
|
 | American Dog Tick
|
 | Brown Dog Tick
|
 | Groundhog Tick
|
 | Gulf Coast Tick
|
 | Rocky Mountain Wood Tick
|
 | Soft Tick
|
 | Western Blacklegged Tick
|
Ticks that commonly bite humans:
Disclosure: We are an Amazon Associate. Some links on this website are affiliate links, which means we may earn a commission or receive a referral fee when you sign up or make a purchase through those links.























Leave a Reply