Despite its name, it’s not actually caused by a worm. The name ‘ringworm’ comes from the ring-like appearance of its symptoms. This condition can cause red spots and itching, which can be quite bothersome. However, there are over-the-counter medications available that can help treat it.
Symptoms
The symptoms of ringworm may include:
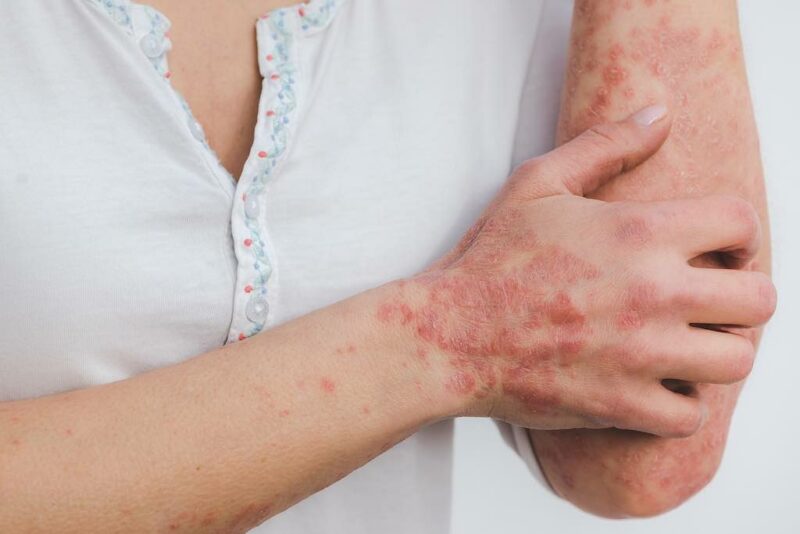
- Formation of scaly ring-shaped areas, usually appearing on the buttocks, torso, arms, and legs.
- Itching.
- Clear or scaly areas inside the ring, which may also have small bumps that can range in color from red to purplish-red, brown, or gray.
- Slightly raised, extended or overlapping rings.
- Round, flat patches of itchy skin.
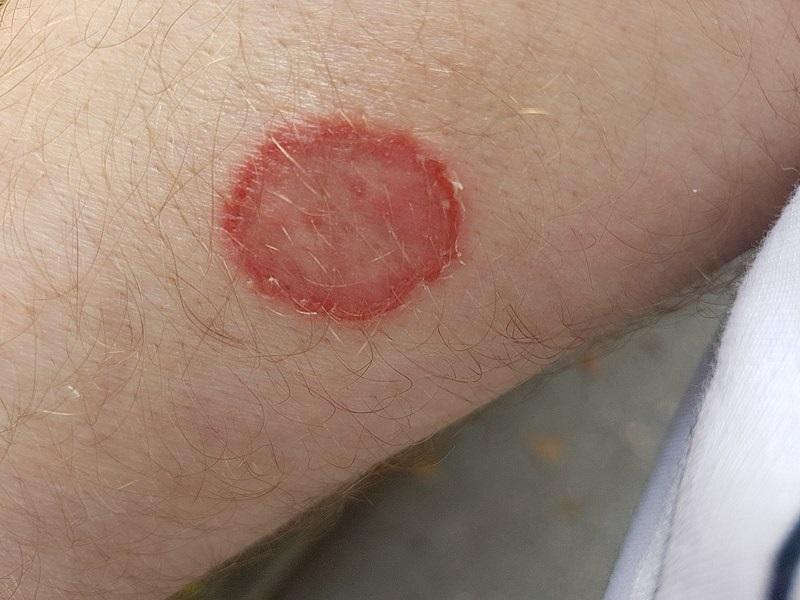
If your ringworm doesn’t start to improve after using over-the-counter antifungal products for two weeks, it’s time to see a doctor. You may need a stronger prescription medication.
Causes
Ringworm is a contagious fungal infection, caused by common mold-like parasites. Yes, it can spread! Here’s how:
- From people to people. Ringworm often spreads through direct skin contact.
- From animals to people. You can get ringworm by touching animals that have it. Petting or grooming dogs or cats can spread ringworm from them to you. It’s also quite common in cows.
- From objects to people. Ringworm can spread by touching objects or surfaces that an infected person or animal has recently touched or rubbed, such as clothing, towels, bedding and linen, combs, and brushes.
- From soil to people. In rare cases, ringworm can spread to people by touching infected soil. But this usually only happens if you’re in contact with highly infected soil for a long time.
If you have unexplained red spots on your body, and some of the symptoms mentioned above, think about whether you have been in contact with people, animals, or objects with suspected symptoms. If so, you probably have ringworm!
Fungi thrive in warm and humid conditions, and certain groups of people in specific environments are more likely to get ringworm. Your risk of getting ringworm increases if you:
- Live in tropical areas.
- Spend a long time in hot, humid weather.
- Sweat a lot.
- Wrestle, play football, or participate in other sports involving contact with others.
- Live closely with others, such as in a barracks.
- Share towels, clothes, razors, and other items without disinfecting (razors) or washing (clothes and towels).
- Are obese.
- Have diabetes.
- Wear clothes that rub against the skin.
- Don’t wash and dry your feet well before putting on shoes and socks in changing rooms or swimming pools.
Treatments
As for treatment, it depends on where the infection is. Mild ringworm can usually be treated by applying topical antifungal medications. For more severe infections, you may need to take antifungal medications for several weeks.
Azoles
Azoles are some of the most commonly used antifungal drugs. They interfere with an enzyme that is important for the fungal cell membrane, destroying the cell membrane and thus killing the fungal cells. There are two subgroups of azole antifungal drugs: imidazoles and triazoles.
Examples of imidazole antifungal drugs and the diseases they treat include:
- Ketoconazole: Infections of the skin and hair, Candida infections of the skin and mucous membranes, blastomycosis, histoplasmosis.
- Clotrimazole: Infections of the skin and mucous membranes.
- Miconazole: Infections of the skin and mucous membranes (including fungal vaginitis).
Some examples of triazole drugs and the diseases they treat are:
- Fluconazole: Candida infections, including mucosal, systemic, and invasive infections; cryptococcosis.
- Itraconazole: Aspergillosis, zygomycosis, histoplasmosis, mucosal Candida infections, sporotrichosis (off-label), and onychomycosis.
- Posaconazole: Aspergillosis (off-label treatment), mucosal and invasive Candida infections.
- Voriconazole: Pneumocystis pneumonia, mucosal or invasive Candida infections, Fusarium infections.
- Isavuconazole: Pneumocystis pneumonia and mucosal diseases.
Polyenes
Polyenes work by making the fungal cell wall more porous, thereby making the fungal cells prone to rupture and killing them.
Some examples of polyene antifungal drugs are:
- Amphotericin B: Various formulations can be used to treat aspergillosis, blastomycosis, cryptococcosis, histoplasmosis (off-label), mucosal or invasive Candida infections, and coccidioidomycosis.
- Nystatin: Candida infections of the skin and mouth.
Allylamines
Like azole antifungal drugs, allylamine drugs interfere with an enzyme involved in creating the fungal cell membrane. An example of an allylamine drug is terbinafine, which is commonly used to treat fungal infections of the skin.
Echinocandins
Echinocandins are a newer type of antifungal drug. They inhibit an enzyme involved in the creation of the fungal cell wall.
Some examples of echinocandin drugs are:
- Anidulafungin: Mucosal and invasive Candida infections.
- Caspofungin: Mucosal and invasive Candida infections, aspergillosis.
- Micafungin: Mucosal and invasive Candida infections.
Ringworm treatments in different areas
Athlete’s foot (Tinea pedis): It can usually be treated with over-the-counter topical antifungal products. Chronic or extensive athlete’s foot may require the use of systemic antifungal drugs such as terbinafine, miconazole, itraconazole, or fluconazole. And if it’s a stubborn chronic case, you might need to add in some extra help like foot powders or talcum powder to keep your skin from getting too soggy.
Scalp ringworm (Tinea capitis): You’re going to need systemic antifungal drugs for this, because the topical stuff just doesn’t cut it. A lot of experts think griseofulvin is the way to go. Terbinafine is also an option, and it’s even got the FDA’s stamp of approval for treating scalp ringworm in patients 4 years old and up. Itraconazole and fluconazole are safe and effective too, but the FDA hasn’t given them the green light for this use yet. You can also use selenium sulfide shampoo as a sidekick in your treatment. Doctors should usually use laboratory tests to confirm the diagnosis of scalp ringworm.
Body ringworm/Jock itch (Tinea corporis/cruris): These can usually be handled with topical antifungal products, and the same stuff you use for athlete’s foot can work here too. If you’ve got groin ringworm, keep that area clean and dry, and stick to cotton underwear. If the infection is widespread or keeps coming back, you might need to go for systemic antifungal therapy.
Most of the time, body ringworm infections get better after antifungal treatment. But sometimes, things don’t go as planned. Treatment might not work if you’ve misdiagnosed yourself or if you stop treatment too soon. Doctors should instruct patients on the importance of taking antifungal drugs as prescribed.
Preventive measures
- Stay clean: Wash your hands frequently, keep shared areas clean, especially in schools, childcare centers, gyms, and locker rooms.
- Stay cool and dry: Do not wear heavy clothing for long periods in warm, humid weather. Avoid excessive sweating.
- Avoid contact with infected animals: Infections usually look like patches of skin missing hair. If you have pets or other animals, have your vet check them for ringworm.
- Do not share personal items: Do not share your clothes, towels, hairbrushes, sports gear, or other personal items. And don’t borrow these items from others either.
Disclosure: We are an Amazon Associate. Some links on this website are affiliate links, which means we may earn a commission or receive a referral fee when you sign up or make a purchase through those links.
















Leave a Reply